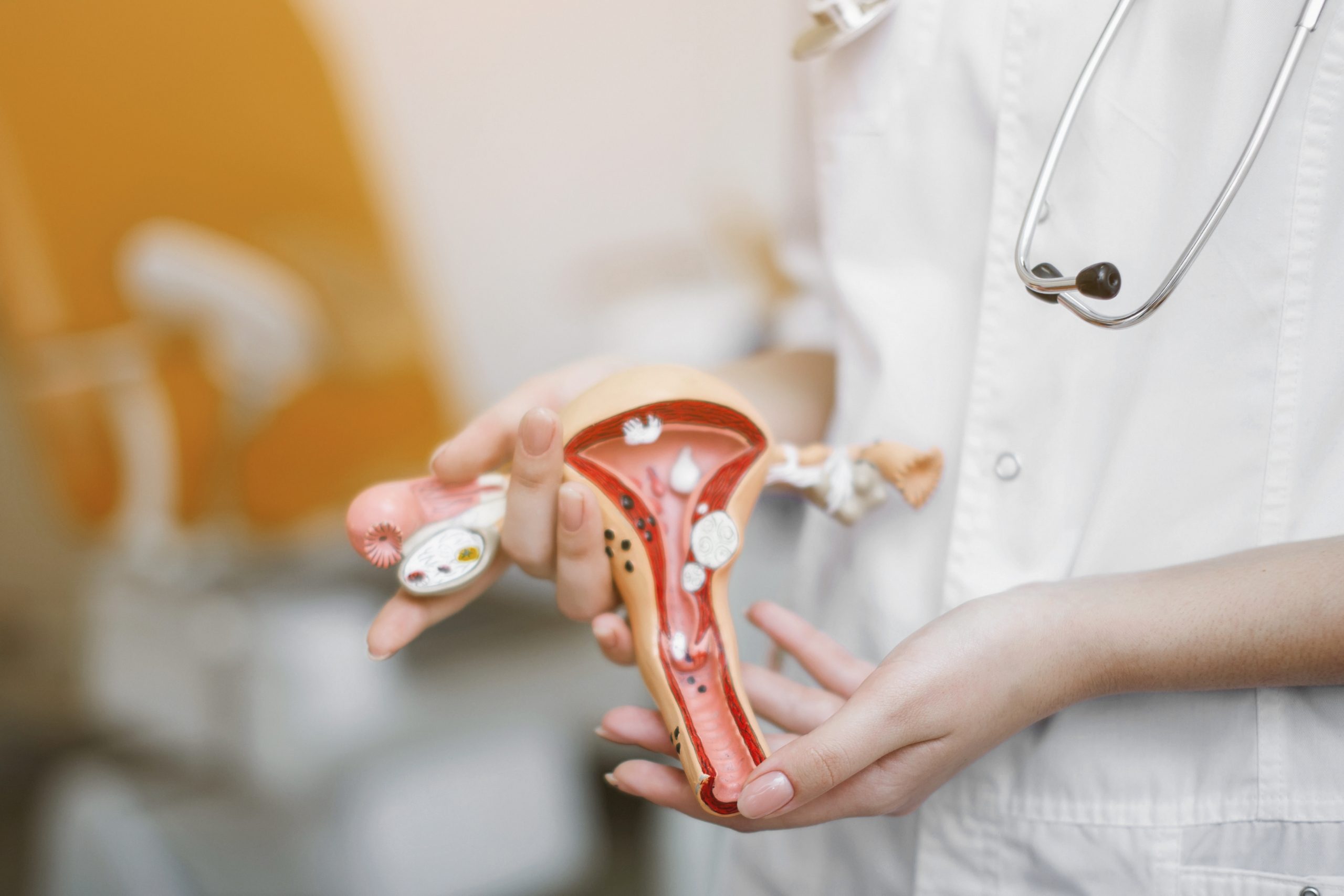
Uterine and Ovarian Inflammations
The realm of gynecological diseases encompasses a wide array of conditions, each bringing its own set of challenges for those affected. Navigating this extensive list and accurately identifying symptoms can be quite a feat. This article is designed to provide you with clarity on the matter. Here you will gain insights into uterine and ovarian inflammation – understanding their origins, symptoms, and available treatment options.
Inflammation is a term you might be familiar with, often associated with the body’s defensive response when invaded by pathogens. However, these inflammatory reactions can also manifest within the internal female reproductive organs, such as the uterus and ovaries, triggered by the intrusion of harmful agents. While instances of these types of inflammations are relatively infrequent in industrialized countries, occurring in about 1% of cases, they typically present with mild symptoms and are amenable to treatment. Understanding the circumstances that trigger inflammatory responses, recognizing key signs that should raise your concern if you are experiencing symptoms, and exploring potential therapeutic approaches are crucial aspects we will ll delve into [1],[2].
Causes of Uterine and Ovarian Inflammation
The uterus and ovaries, together with the fallopian tubes and cervix, constitute the upper female genital tract. Inflammations affecting these internal female genital organs are primarily triggered by ascending infections. These occurrences are more prevalent among women aged 15 to 24. The main causative pathogens for ascending infections include [2],[3]:
- Gonococci
- Chlamydia
- Streptococci
- Staphylococci
- Ureaplasma
- Coliform bacteria
Approximately 85% of cases of upper genital tract inflammations result from ascending infections caused by sexually transmitted bacteria: notably gonococci and chlamydia. Gonococci typically produce more severe symptoms, while chlamydia often induces few or no noticeable symptoms initially. Chlamydia usually affects the urinary tract first, causing urethritis, which can be asymptomatic in the early stages, leading to potential missed diagnosis and treatment. This can facilitate the upward propagation of the inflammatory reaction to the vagina and upper genital tract. Gonococci are responsible for gonorrhea, a sexually transmitted disease that can ascend from the vagina to the upper genital organs. Streptococci, staphylococci, ureaplasmas, and coli account for approximately 15% of ascending infection cases [4],[5],[6],[7].
In addition to ascending infections, descending infections can also contribute to uterine and ovarian inflammation, albeit rarely. Descending infections involve pathogens that move from neighboring organs to internal reproductive organs like the ovaries and uterus. The transmission can occur through direct contact or via the lymphatics. For example, appendicitis can lead to the spread of inflammation. Furthermore, pathogens can enter the uterus and ovaries through hematogenous infection, causing inflammation to spread. Tuberculosis pathogens, for instance, can cause inflammatory processes within internal reproductive organs. [8]
Infection is more likely when your natural protective mechanisms are compromised. The vagina and cervix play pivotal roles in the female genital tract’s natural defense mechanism. The vagina’s acidic environment ordinarily inhibits harmful germ proliferation, while the cervix forms an effective barrier through cervical mucus. Under special conditions, however, these protective mechanisms can be breached more easily, rendering the body susceptible to inflammation of internal genital organs. Contributing factors include [9]:
- The first years after puberty: During this period, the vaginal and cervical mucosal cell layer is thinner and more vulnerable, allowing germs to penetrate more readily.
- A dry or alkaline vaginal environment: Such conditions facilitate the colonization and proliferation of harmful microorganisms like bacteria and fungi.
- Pathological changes in the cervix and uterus: Conditions like endometrial carcinoma (uterine cancer), and benign tumors (myomas, polyps), can increase mucous membrane permeability in the cervix and uterus.
- Estrogen deficiency: Menopause-induced lower estrogen levels cause the uterine lining to become drier and thinner, diminishing its protective function. This form of uterine inflammation is also termed endometritis senilis.
- Foreign bodies: Inserted foreign bodies like IUDs increase the risk of germ spread.
- Surgical vaginal procedures: During IUD insertion, uterine scraping, or endoscopy, cervical dilation allows germs to be transported into the uterus more easily.
- Menstruation: During menstruation, the slightly open cervix can facilitate germ entry.
- Abortion: Retention of pregnancy products following an abortion can lead to inflammation.
- Childbirth: The cervix remains slightly open and permeable for 6–8 weeks after childbirth, making it easier for germs to enter the uterus. Additionally, the body’s defenses are weakened after childbirth, making it more susceptible to bacteria. Afterbirth remnants in the uterus can also cause inflammation. Postpartum fever, wherein pathogens spread via the bloodstream, posing a risk of blood poisoning, can occur after childbirth. This uterine inflammation is known as postpartum endometritis. The likelihood of postpartum endometritis depends on the delivery mode, occurring in 1-3% of vaginal deliveries, 5-15% of planned cesarean sections, and 15-20% of unplanned cesarean sections [8],[10],[11].
Aside from these circumstances, other risk factors can contribute to uterine and ovarian infection development, such as being under 25, having new or multiple sexual partners, and engaging in unprotected sexual activity [14],[15].
Understanding the ascending spread of inflammation and the consequences of germ propagation involves considering the anatomy of female internal reproductive organs, including the vagina, cervix, uterine cavity, ovaries, and fallopian tubes. Any of these organs can be affected by inflammation.
Visualize ascending infections in the female genital tract as follows: Pathogen entering the vagina causes vaginitis. As the infection advances, cervicitis or inflammation of the cervix can ensue. Following this progression, the inflammation can advance to affect the uterine wall, which consists of distinct layers [8]:
- Endometrium: The innermost layer and lining of the uterus
- Myometrium: The muscular layer
- Perimetrium: The outermost layer, also known as the peritoneum [12],[13].
When inflammation targets the endometrium, it is termed endometritis. If the inflammation, extends to the uterine muscles, it is referred to as myometritis. If the infection remains untreated and spreads unchecked, it can progress from the vagina to the uterus. Consequently, inflammation can extend to the ovaries (oophoritis) and fallopian tubes (salpingitis). Often ovarian and fallopian tube inflammation coexists, carrying the medical term adnexitis. [14]
As you can observe, anatomically, the infection ascends from the “lower” regions (vagina), traversing the cervix and uterus, and propagates to the “higher” regions of the fallopian tubes and ovaries.
In the realm of medicine, these inflammations of the upper female genital tract (cervicitis, endometritis, and adnexitis) are collectively classified as “Pelvic Inflammatory Diseases (PID)“. PID typically manifests as a combination of these inflammatory conditions and can lead to intricate inflammatory responses. [8]
What are the Possible Symptoms of Uterine and Ovarian Inflammation?
Having delved into the progression of endometritis, cervicitis, and adnexitis, let us explore the potential symptoms that individuals may experience and how they can be differentiated.
The symptoms associated with these conditions can often be nonspecific, varying depending on the stage of inflammation and the parts of the upper genital tract affected.
In cervicitis, symptoms are typically mild and may include:
- Increased or discolored discharge (ranging from white-yellow to reddish-bloody), often accompanied by a strong odor.
- Sensation of burning and itching in the vaginal area [15],[16].
As endometritis develops, with inflammation extending to the endometrium and/or to the uterine muscles, additional symptoms might emerge:
- Pressure-related pain in the region of the uterus.
- Possibility of bleeding and menstrual irregularities, such as heavy, prolonged, or irregular periods, as well as spotting [3], [11], [17].
When adnexitis occurs, with inflammation affecting the fallopian tubes and/or ovaries, more pronounced symptoms may arise:
- Noticeable malaise.
- Often sudden and severe lower abdominal pain, which can occur on the left, right, or frequently on both sides.
- Abdominal wall that feels tense, bulging, and hard.
- Fever, accompanied by nausea and vomiting.
- Altered vaginal discharge, frequently purulent.
- Unusual vaginal bleeding.
- Pain during sexual intercourse [18],[19].
In terms of the course of the illness, a distinction can be made between acute and chronic inflammation. Chronic endometritis, or adnexitis refers to ongoing inflammation of the endometrium/fallopian tubes and ovaries. Such cases are often mild, asymptomatic, or even display no symptoms at all. They commonly arise due to untreated acute inflammation or from scarring changes and adhesions following treated inflammation.
The symptoms associated with chronic inflammation typically encompass:
- Unspecific pain in the lower back and pelvic floor.
- Recurring, dull lower abdominal pain of varying intensity, which may increase when sitting or engaging in physical activities.
- Frequent fatigue.
- Tendency towards a depressive mood.
- Symptoms such as constipation, bloating, pain, and in rare cases abnormal menstruation [19],[20],[21].
Chronic inflammation may also contribute to infertility. A study indicates that successful birth rates among women without chronic endometritis stand at 85%, whereas the rate among those with untreated endometritis is 68%. Encouragingly, chronic endometritis can respond well to antibiotic treatment, enhancing the outlook for a subsequent successful pregnancy [1].
What are the Treatment Options?
When it comes to treating inflammations of the upper female genital tract, a range of options is available. The choice of treatment depends on the specific cause of inflammation and the pathogen involved. For cases where bacterial infection is identified, antibiotic therapy is a common approach for cervicitis, endometritis, and adnexitis. Typically, antibiotics like ciprofloxacin, cephalosporin, doxycycline, and metronidazole are prescribed to eliminate the pathogens. [23],[24],[25]
In more severe instances, particularly in cases of postpartum inflammation, clindamycin, and gentamycin antibiotics are often employed. Additionally, if inflammation arises after childbirth, the hormone oxytocin is administered alongside antibiotics. This hormone assists in uterine contractions and the subsequent shedding of the inflamed endometrium. If inflammation results from placental remnants in the uterus, curettage might be performed after symptoms subside to prevent reoccurrence. Hormone replacement therapies involving estrogen and progestin can be considered for menopausal inflammation over a 20-day period to counter declining estrogen levels [24],[25].
For symptom relief, analgesic therapy is frequently recommended, following consultation with a medical professional. Bed rest is advised for affected individuals to prevent undue strain on the body. Sexual intercourse should be avoided until the infection has cleared, and the sexual partners of affected individuals should also seek treatment from a doctor. Depending on symptom severity, inpatient therapy might be considered. For instance, if infection leads to fever and nausea and ultrasound reveals abnormalities, hospital treatment may be necessary. In cases where pus is found in the uterus, surgery under general anesthesia could be required to disinfect and flush the uterine cavity. If inflammation is linked to a foreign object, such as an inserted IUD, removal might be necessary in certain situations [26].
The overview of uterine and ovarian inflammation underscores the interconnectedness of these conditions. Causes and pathogens can typically be identified, and tailored therapies are available based on the nature of the inflammation. What can you do if you experience any of the symptoms mentioned, or suspect inflammation? It is important to be vigilant and observant. Every symptom should be taken seriously and assessed. If you suspect inflammation, the next step is to consult a gynecologist to determine possible pathogens and classify causes and symptoms. This approach is essential for establishing an accurate diagnosis and implementing appropriate treatment.
The Endo-App offers you the opportunity to track your daily wellbeing.
By clicking the button below, you can access the Endo-App, now available for free for those affected.
References
- Lax, S.F. Endometritis. Pathol: https://doi.org/10.1007/s00292-016-0237-x, called on 14 November 2022.
- Anvil: inflammations of the female genital tract: https://www.amboss.com/de/wissen/Entzündungen_des_weiblichen_Genitaltrakts/, accessed November 14, 2022.
- Singh N, Sethi A. Endometritis – Diagnosis,Treatment and its impact on fertility – A Scoping Review. (2022): [4] https://pubmed.ncbi.nlm.nih.gov/35621273/, called at 14 November 2022.
- S2k guideline: Infections with Chlamydia trachomatis, German STI Society – Society for the Promotion of Sexual Health: https://register.awmf.org/de/leitlinien/detail/059-005, accessed November 14, 2022.
- Molenaar MC, Singer M, Ouburg S. The two-sided role of the vaginal microbiome in Chlamydia trachomatis and Mycoplasma genitalium pathogenesis. J Reprod Immunol; 2018.
- Di Tucci C, Di Mascio D, Schiavi MC, Perniola G, Muzii L, Benedetti Panici P. Pelvic Inflammatory Disease: Possible Catches and Correct Management in Young Women. Case Rep Obstet Gynecol; 2018.
- Risser WL, Risser JM, Risser AL. Current perspectives in the USA on the diagnosis and treatment of pelvic inflammatory disease in adolescents. Adolesc Health Med Ther; 2017Online information of the Professional Association of Gynecologists (BVF): PID: https://www.frauenaerzte-im-netz.de/erkrankungen/adnexitis-salpingitis-pelvic-inflammatory-disease/ursachen-und-risikofaktoren/#c849, accessed November 15, 2022.
- Online information of the Professional Association of Gynecologists (BVF): Uterine inflammation: Causes: https://www.frauenaerzte-im-netz.de/erkrankungen/gebaermutterentzuendung/ursachen/, accessed November 15, 2022.
- MSD Manuals: Endometritis puerperalis: https://www.msdmanuals.com/de-de/profi/gynäkologie-und-geburtshilfe/wochenbettpflege-und-begleitende-störungen/endometritis-puerperalis, accessed November 16, 2022.
- Pschyembel: Endometritits: https://www.pschyrembel.de/Endometritis/K06TM/doc/, accessed November 16, 2022.
- Amboss: Uterus: https://next.amboss.com/us/article/O60IOS?q=uterus#Za01eee7dd508a9ffebff19996b63507a, accessed 17 November 2022.
- Uhlig, NM. Anatomie der Gebärmutter: https://www.fernarzt.com/anatomie/gebaermutter/, accessed 15 November 2022.
- Pschyrembel: Inflammatory disease: https://www.pschyrembel.de/Pelvic%20Inflammatory%20Disease/K00VS/doc/, accessed 17 November 2022.
- Pschyrembel: Zervizitis: https://www.pschyrembel.de/Zervizitis/K0PC6/doc/, accessed 18 November 2022.
- Netdoktor: Tiefenböck F, Feichter M. Chlamydien: https://www.netdoktor.de/krankheiten/chlamydien-infektion/, accessed 18 November 2022.
- Dr. Gumpert: Gumpert N. Unterleibentzündung: https://www.dr-gumpert.de/html/entzuendung_unterleib.html, accessed 18 November 2022.
- Pschyembel: Adnexitis:https://www.pschyrembel.de/Adnexitis/K01QD/doc/, accessed 18 November 2022.
- Netdoctor: Feichter M. Fallopian tube inflammation and ovarian inflammation: https://www.netdoktor.de/krankheiten/eileiterentzuendung-und-eierstockentzuendung/, accessed 18 November 2022.
- Kitaya K, Takeuchi T, Mizuta S, Matsubayashi H, Ishikawa T. Endometritis: new time, new concepts. Fertil Steril 2018;110: 344–50.
- Fertility Blog: Schuff M. Chronische Endometritis: https://www.kinderwunsch-blog.com/chronische-endometritis-fakt-oder-fiktion/, accessed 18 November 2022.
- Netdoctor: Feichter M. Fallopian tube inflammation and ovarian inflammation: https://www.netdoktor.de/krankheiten/eileiterentzuendung-und-eierstockentzuendung/, accessed 18 November 2022.
- Jennings LK, Krywko DM. Pelvic Inflammatory Disease. https://www.ncbi.nlm.nih.gov/books/NBK499959/, accessed 18 November 2022.
- Mackeen AD, Packard RE, Ota E, Speer L. Antibiotic regimens for postpartum endometritis. Cochrane Database of Systematic Reviews 2015, Issue 2. Art. No.: CD001067. DOI: 10.1002/14651858.CD001067.pub3, accessed 18 November 2022.
- Amboss: Endometritis: https://next.amboss.com/us/article/Ek08pT#Zf8e1decd77cd3c6b37f3d2ffebf3dbba, accessed 18 November 2022.
- MSD Manuals: PID: https://www.msdmanuals.com/de-de/profi/gynäkologie-und-geburtshilfe/vaginitis-zervizitis-und-pelvic-inflammatory-disease/pelvic-inflammatory-disease-pid, accessed 1 9 November 2022.
Do you have any comments or questions about uterine and ovarian infections?
Feel free to leave us a comment.
- Investigating the Effects of Green Tea Complex or Extract on Pain and Mucosal Health - 1. October 2023
- Understanding Primary Dysmenorrhea: Causes, Symptoms, and Treatment - 26. September 2023
- Why is Endometriosis So Often Mistaken for Chlamydia? - 2. September 2023