Endometriosis often leads to chronic pain, bowel problems and also pelvic floor tension. Therefore, osteopathy is sometimes recommended as an additional option as part of a multimodal therapy.
Many women report good results. Even though large studies are lacking, there are small ones that give hope! They indicate that osteopathy can relieve discomfort and symptoms.
1. What is Osteopathy?

Osteopathy
Osteopathy, a relatively modern medicinal discipline, was developed in the 19th century by Andrew Still.
Central to osteopathy is a dedicated emphasis on the fascia – thin layers of connective tissue that envelop muscles, organs, and various bodily structures. Concurrently, these connective tissue layers interweave, forming a cohesive unit known as the body fascia [3].
The primary objective of osteopathy lies in identifying and addressing obstructions or limitations in the movement of the body’s fascia, with the ultimate goal of reinstating optimal bodily function. The extent of research findings varies based on the specific condition under scrutiny.
Osteopathy, recognized as a medical discipline, is a practice exclusive to licensed physicians and qualified alternative practitioners. It is frequently applied within the realm of orthopedics and can also complement the management of chronic ailments. Within this discipline, two noteworthy branches exist: muscular osteopathy and visceral osteopathy. The latter is attuned to the internal organs and holds particular relevance for women dealing with endometriosis.
When it comes to the abdominal region, osteopaths focus on rectifying normal function and mobility of organs by addressing tensions in the connective tissues. This encompasses addressing issues like adhesions between organs as well as treating scars.
2.Effect on Endometriosis and Pelvic Floor Tension

Enhancing pelvic floor function with osteopathy.
Studies have revealed a notable correlation between chronic lower abdominal pain and heightened pelvic floor tension among women. Furthermore, this discomforting tension appears to be more prevalent in those affected by endometriosis [6].
A gynecologist can discern these tensions through vaginal examination. In instances of endometriosis, pelvic floor tensions can arise as a response to the discomfort experienced. However, paradoxically, these tensions can also fuel self-sustaining pain.
Such pelvic floor tension can contribute to cramping discomfort in the lower abdomen and generate pain during activities like intercourse, urination, or bowel movements.
While treatment focused solely on spinal manipulation exhibited no discernible effect on menstrual cramps [5], alternative osteopathic techniques have demonstrated more promising outcomes [1,2,7,8].
In a study encompassing 28 participants, significant pain alleviation was observed among individuals contending with chronic lower abdominal pain and pelvic floor tension [7].
Encouragingly, the most pronounced improvement occurred among women grappling with endometriosis and pelvic floor tension. Remarkably, 71% of women (10 out of 14) experiencing both endometriosis and pelvic floor tension reported symptom improvement following osteopathic treatment [7].
Additionally, studies have highlighted favorable outcomes in the realm of back pain and bladder-related issues.
3. Effect on Deep Infiltrating Endometriosis
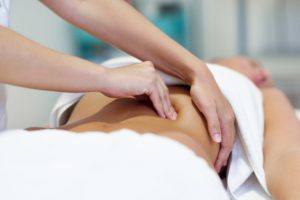
Osteopathy on the abdomen aims to improve the mobility of the muscles but also of the organs (especially the intestines).
Osteopathy is centered on restoring the mobility of internal organs through the relaxation of connective tissues.
In endometriosis, particularly in cases of deep infiltrating endometriosis, organ mobility becomes restricted due to the presence of endometriosis lesions and the subsequent development of adhesions. Surgical procedures can also contribute to the formation of adhesions.
Among the vital organs reliant on mobility for proper functioning, the intestine stands out. A study conducted in France examined the impact of osteopathy on women afflicted by rectal endometriosis (colorectal endometriosis).
The study encompassed 46 patients who received osteopathic treatment, and the resultant effects on their quality of life and symptoms were scrutinized. The findings, following a month of consistent osteopathy sessions, showcased a distinct positive impact [1].
Osteopathy was found to improve:
- Gynecological symptoms
- Digestive symptoms
- General well-being
- Psychological state
- Overall quality of life [1].
Furthermore, in a small-scale study, the benefits of abdominal massage treatment were still evident six weeks post-treatment, with participants reporting sustained reductions in pain levels compared to their pre-study experiences [8].
The enhancement of quality of life is likely a direct consequence of the mitigation of pain, given that pain is frequently perceived as the foremost challenge and the underlying cause of numerous limitations.
4. Which Osteopathic Treatment is Right for Me?
Within the studies, osteopathic interventions encompassed treatments applied to the abdomen, diaphragm, lower back, and, naturally, specific points based on the specific complaints presented.
Certain osteopaths provide the Touché technique as a prospective solution for menstrual pain, involving intravaginal massage. However, it is vital to note that no scientific findings exist in this regard, thereby hindering any definitive conclusions. The outcomes discussed in this context do NOT involve the Touché technique. Hence, a conventional osteopathic treatment is expected to be ample for the intended outcomes.
Conclusion
Regrettably, the body of research examining the relationship between osteopathy and endometriosis remains limited. Nevertheless, the existing studies and accounts from women with endometriosis have illuminated a pain-alleviating and positive effect. Osteopathic interventions, such as those targeting the abdomen and back, have garnered recognition from prominent figures in the field of endometriosis, including respected specialists like Prof. Dr. Sylvia Mechsner. These professionals consider osteopathy a potentially valuable component within the broader scope of endometriosis therapy [9].
For women afflicted by endometriosis, pelvic floor tension frequently engenders considerable pain. The relaxation of these tense areas through both physical therapy and osteopathy has demonstrated the potential to provide relief. It is noteworthy that osteopathy holds the promise of reducing pain and enhancing the overall quality of life for women beyond those affected by endometriosis.
Osteopathy should be especially considered by individuals dealing with deep infiltrating endometriosis, pelvic floor tension, urinary issues, gastrointestinal problems, or back pain. Naturally, it is essential to recognize that osteopathy should always be regarded as a complement to gynecological therapy.
Given the existing scarcity of comprehensive research, each person is encouraged to assess individually whether osteopathy proves beneficial for their specific concerns. However, the current state of data provides a hopeful outlook.
References
- “Take yourself and your endometriosis seriously. You are not imagining things!” - 5. November 2023
- Increased Risk of Stroke Due to Endometriosis - 4. October 2023
- Does Monk’s Pepper Help with Endometriosis? - 24. September 2023

Your comprehensive exploration into osteopathy’s potential in treating endometriosis is both enlightening and promising. It’s intriguing to see how a practice rooted in the 19th century can find relevance in addressing contemporary medical concerns like endometriosis. The article skillfully underscores the connection between bodily fascia, pelvic floor tension, and endometriosis. By considering both disciplines, we can emphasize the significance of integrated care approaches in optimizing patient outcomes.