Endometriosis in the Brain
Endometriosis, a condition in which tissue resembling the uterine lining grows outside the uterus, leads to tissue islands known as endometriosis lesions. These lesions mimic the behavior of the endometrium and, in sync with the menstrual cycle, accumulate and eventually shed. In a typical scenario, the endometrium is shed through the vagina during menstrual bleeding. However, in the case of endometriosis, these lesions trigger inflammation and pain. Moreover, the persistence of this ectopic tissue can give rise to adhesions or cysts [1]. Endometriosis commonly affects the pelvis, ovaries, and urinary bladder. Remarkably, it can also manifest in the brain [2].
Today, we will delve into what these occurrences mean for patients, their implications for understanding the development of endometriosis, and the various treatment approaches.
Locations of Endometriosis Lesions
Endometriosis lesions can manifest in various locations, leading doctors to distinguish between different forms of the condition based on their location and spreading pattern:
- Peritoneal Endometriosis: In this form, endometriosis foci are found within the abdominal cavity [2].
- Ovarian Endometriosis: This variant affects the ovaries, with stray endometrial tissue impacting these reproductive organs [2].
- Adenomyosis Uteri: This type presents with endometrial glands and supporting stomatal cells in the uterine muscles, where they are not typically found. This can result in the enlargement of the uterus [2, 3].
- Deep Infiltrating Endometriosis: Here, endometriosis lesions penetrate beyond the surface, infiltrating nearby tissues and organs to a depth of at least 0.5 cm [4].
- Endometriosis Extragenitalis: In this form, endometriosis tissue extends beyond the genital tract, potentially leading to mucosal deposits in areas such as the intestine, diaphragm, urinary bladder, and even the lungs. Although rare, endometriosis can also affect the brain [2].
Today, our focus will be on endometriosis extragenitalis.
Endometriosis in the Brain: Uncommon yet Feasible
In gynecological diseases, endometriosis takes the second spot, just after fibroids. It is estimated that 5-10% of women of childbearing age are affected by the condition [5]. However, endometriosis lesions in the brain are a true rarity. Such occurrences are incredibly infrequent, and there is a lack of precise statistics on their prevalence. Knowledge about the associated symptoms remains limited since only individual cases have been reported. In these reports, endometriosis has been linked to neurological symptoms, affecting the nervous system. They encompass headaches, seizures, or even loss of consciousness [6].
Given the non-specific nature of these symptoms, which can result from numerous other, more common causes, diagnosing endometriosis in the brain primarily involves ruling out other potential explanations.
It is worth noting that cyclic headaches can occur independently of endometriosis.
The typical endometriosis symptoms can also be in the foreground and include [5]:
- Abdominal pain
- Feeling of fullness
- Nausea
- Menstrual irregularities
- Infertility
- Back pain
- Pain during sexual intercourse
Good to Know!
Endometriosis is commonly diagnosed during a woman’s childbearing years, particularly between the ages of 20 and 40. This is due to the influence of hormonal regulation on the menstrual cycle, which plays a role in the development of endometriosis lesions and associated symptoms. It is worth noting that not all patients with endometriosis experience noticeable symptoms. Only 65% of all patients report them [5]. As a result, endometriosis can often go undetected for an extended period.
How Endometriosis Lesions Reach the Brain
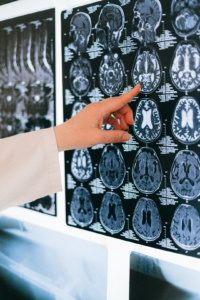 The journey from the uterus to the brain is a pretty remarkable one. This raises the question of how endometriosis lesions enter the brain. Various theories attempt to shed light on this intriguing phenomenon. Let us explore these assumptions together.
The journey from the uterus to the brain is a pretty remarkable one. This raises the question of how endometriosis lesions enter the brain. Various theories attempt to shed light on this intriguing phenomenon. Let us explore these assumptions together.
- Retrograde Menstruation: Menstrual bleeding does not solely exit the vagina, as often believed. It can also enter the abdominal cavity through the fallopian tubes, potentially allowing endometrial cells to settle there. While this theory seems logical, it does not explain why not all women develop endometriosis during menstruation [5, 7].
- Altered Epithelial Cells: Another theory suggests that changes in the epithelial cells on the surface of the peritoneum may support the development of endometriosis. This theory is based on the shared origin of epithelial and endometriosis cells [6].
- Metaplasia of Embryonic Remnants: This theory delves into the transformation of embryonic remnants from the Müller duct. The Müller duct is a standard embryonic structure in both sexes, responsible for developing the female reproductive organs, including the vagina, uterus, and fallopian tubes [5]. Researchers speculate that endometriosis may involve the transformation of these embryonic remains from the Müller ducts [5, 6].
- Abnormalities in the Immune System: The immune system’s role in endometriosis has garnered attention. A misdirected immune cell response may contribute to the development of endometriosis [6].
- Transport by the Blood and Lymphatic Systems: The blood and lymphatic systems are integral to the body’s functioning. The lymphatic system serves a cleansing function, while the blood transports essential nutrients and oxygen and supports the immune system. Fluids are in constant circulation throughout the body. One theory proposes that endometriosis cells could be distributed via the blood-vascular or lymphatic systems [6].
Understanding how endometriosis lesions can reach the brain remains a subject of ongoing research, and these theories provide valuable insights into this complex process.
Diagnosing Endometriosis in the Brain
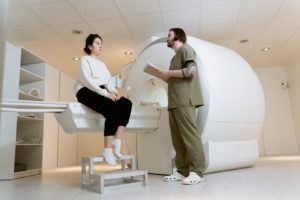
There are several methods for detecting endometriosis. To begin, a comprehensive medical history discussion is essential. This allows the collection of existing symptoms and gives the physician an overview of the patient’s quality of life.
Using a vaginal ultrasound device, endometriosis lesions can be visualized in specific locations, such as between the intestine and the vagina (rectovaginal), when performed by trained examiners. However, it is essential to note that the imaging technique is unsuitable for examining the brain due to the strong reflection of ultrasound waves by bone. If endometriosis in the intestine is suspected, an ultrasound examination through the rectum can be conducted.
A laparoscopy is another diagnostic tool to examine endometriosis lesions closely. It also allows the surgeon to gauge how much these lesions have spread. In cases where tissue is removed during laparoscopy, it can be further analyzed in a laboratory to confirm the diagnosis of endometriosis [5].
However, it is crucial to acknowledge that these measures are not designed to detect endometriosis lesions in the brain. They primarily assess whether the tissue has settled in locations outside the uterus.
For the brain and other organs, an MRI (magnetic resonance imaging) is a reliable tool for revealing endometriosis lesions [9]. It can also help detect mucosal islands in the brain or endometriosis in the lungs. Your physician will discuss the appropriate diagnostic options for your specific case.
Treating Endometriosis Lesions in the Brain
Being an intricate and sensitive organ, the brain calls for surgical interventions only when they are deemed promising and absolutely necessary. When endometriosis lesions are found in the brain, the treating physician must make crucial decisions regarding the next steps.
Often, the initial approach is to explore non-surgical treatment options. One recommended option, as outlined in the guideline of the German Society for Gynecology and Obstetrics, is the use of progestogens, such as Dienogest [2]. Dienogest is a synthetically produced corpus luteum hormone that mimics the action of the body’s natural progesterone. This hormone is believed to counteract an excess of estrogen, a common feature in endometriosis. By doing so, it aims to alleviate symptoms and improve patient prognosis.
Good to Know!
Endometriosis is intricately linked to hormones. Explore the topic in our article “Estrogen and Endometriosis: Exciting Connections.”
In a Nutshell
In endometriosis, there are outlying islands of mucous membrane, also known as endometriosis lesions. These islands are composed of tissue closely resembling the uterus lining. Regrettably, this unwanted growth can give rise to distressing symptoms, including abdominal pain, infertility, and menstrual disorders.
While these growths are frequently observed in the pelvis,
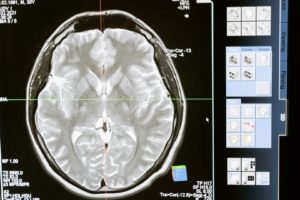 on the ovaries or within the urinary bladder, they can, in rare instances, also manifest in the lungs and even the brain. Endometriosis in the brain is indeed an exceptional occurrence, so research in this area is still in its nascent stages. The mechanisms by which endometriosis cells infiltrate the brain’s command center remain uncertain. One theory suggests these cells may disseminate through the bloodstream and lymphatic system.
on the ovaries or within the urinary bladder, they can, in rare instances, also manifest in the lungs and even the brain. Endometriosis in the brain is indeed an exceptional occurrence, so research in this area is still in its nascent stages. The mechanisms by which endometriosis cells infiltrate the brain’s command center remain uncertain. One theory suggests these cells may disseminate through the bloodstream and lymphatic system.
Diagnostic tools like MRI (magnetic resonance imaging) are particularly well-suited to visualize these changes. Established methods such as progesterone-based drug therapy can be considered when it comes to treatment.
References
- Endometriose | Gesundheitsinformation.de
- German Society of Gynecology and Obstetrics: Guideline Program. Diagnosis and therapy of endometriosis. August 2020.
- Uterine Adenomyose – Gynäkologie und Geburtshilfe – MSD Manual Profi-Ausgabe (msdmanuals.com)
- Koninckx PR, Martin DC. Deep endometriosis: a consequence of infiltration or retraction or possibly adenomyosis externa? Fertil Steril. 1992 Nov;58(5):924-8. doi: 10.1016/s0015-0282(16)55436-3. PMID: 1426377.
- Dietrich, Klaus: Gynaecology and Obstetrics (Springer Textbook) 2nd edition, Springer Verlag.
- Thibodeau LL, Prioleau GR, Manuelidis EE, Merino MJ, Heafner MD. Cerebral endometriosis. Case report. J Neurosurg. 1987 Apr;66(4):609-10. doi: 10.3171/jns.1987.66.4.0609. PMID: 3559727.
- Gibran L, Maranhão RC, Abrão MS, Baracat EC, Podgaec S. Could statins constitute a novel treatment for endometriosis? Systematic review of the literature. Eur J Obstet Gynecol Reprod Biol. 2014 Aug;179:153-8. doi: 10.1016/j.ejogrb.2014.05.028. Epub 2014 Jun 2. PMID: 24965997
- Ms Miriam Szabo, Ms Lisa Buck, Dr Adam Steel, Prof Christian M. Becker, Prof Katy Vincent. Volumetric Changes in the Brains of woman with Endometriosis-associated pain are dynamic. Presentation at World Endometriosis Congress 2021.
- Schonende Diagnose der Endometriose – MRT spürt Schleimhautinseln auf | DRG.de
- Pharmaceutical Companies and Their Influence on Scientific Research - 7. October 2023
- Identification of a Genetic Factor Linked to Endometriosis Development and Potential Therapeutic Targets - 6. October 2023
- Identification of a Genetic Factor Linked to Endometriosis Development and Potential Therapeutic Targets - 6. October 2023
