Autoimmune Conditions and Endometriosis: Study Proves a Connection
Endometriosis is a chronic gynecological condition that commonly affects up to 15% of women of childbearing age [1]. Historically, it was believed to impact the abdominal cavity primarily and, in most cases, only the pelvic region. However, recent research indicates it is a systemic condition [2]. While the precise causes of endometriosis remain elusive, immune system irregularities are evident. A meta-analysis explored the link between endometriosis and autoimmune conditions [3]. Although additional comprehensive studies are needed to supplement existing research, substantial evidence suggests a close connection between endometriosis and the immune system.
Symptoms of Endometriosis: Beyond Menstrual Pain
Endometriosis is a benign condition characterized by the growth of cell clusters resembling the uterine lining, or endometrium, outside the uterus [4]. These cell clusters, known as endometriosis lesions, can manifest in various locations, including the muscular layers of the uterine wall, the vagina, the peritoneum, the urinary bladder, and the ureter. Additionally, they can affect the intestines, lungs, liver, and skin scars.
Traditionally, endometriosis has been associated with cyclic lower abdominal pain that may radiate to the back and legs. It is also a recognized contributor to reduced fertility and infertility [5]. However, recent research reveals systemic inflammatory responses and heightened pain sensitization in individuals with endometriosis [6]. Furthermore, a recent study has established a connection between endometriosis and rheumatoid arthritis [7].
Unraveling Endometriosis: Understanding Its Causes and Risk Factors
The precise causes of endometriosis remain elusive despite ongoing research efforts. While multiple theories have been proposed, none comprehensively explain all aspects of the condition [8]. Consequently, experts now believe that endometriosis likely arises from a combination of hormonal, immunological, anatomical, and (epi-)genetic factors.
Some of the critical theories regarding the development of endometriosis include:
- Retrograde Menstruation Theory: This theory suggests that endometrial cells enter the abdominal cavity through the fallopian tubes during menstruation.
- Coelomic Metaplasia Theory: According to this theory, endometriosis lesions develop from cells within the peritoneum, pleura (chest/rib lining), and ovaries.
- Stem Cell Theory: This theory posits that stem cells originating from the bone marrow may be responsible for developing endometriosis lesions.
- Lymphatic/Vascular Benign Metastasis Theory: According to this theory, endometriosis tissue may be transported from the uterus to other body parts through the lymphatic system or blood vessels.
Endometriosis and Autoimmune Conditions: An Overview of the Study and Its Findings
 The 2019 study is classified as a meta-study, which involved comprehensive research and evaluation of existing studies related to the topic. Its primary objective was to determine if the available research findings supported the connection between endometriosis and autoimmune conditions.
The 2019 study is classified as a meta-study, which involved comprehensive research and evaluation of existing studies related to the topic. Its primary objective was to determine if the available research findings supported the connection between endometriosis and autoimmune conditions.
A total of 26 studies adhering to specific criteria were incorporated into this meta-study. These studies collectively provided evidence indicating an association between endometriosis and autoimmune conditions. Subsequently, four studies were chosen in a further selection process. These studies not only met the qualitative standards of the study design but also demonstrated a scientifically significant relationship between endometriosis and autoimmune conditions.
 Among the 4 studies with validated findings, an association between endometriosis and the following autoimmune conditions was identified:
Among the 4 studies with validated findings, an association between endometriosis and the following autoimmune conditions was identified:
- Systemic Lupus Erythematosus: A rheumatic condition primarily affecting the skin and joints, characterized by redness and joint pain.
- Sjögren’s Syndrome: A condition affecting the salivary and lacrimal glands.
 Rheumatoid Arthritis: This autoimmune condition particularly impacts the joints in the hands and feet.
Rheumatoid Arthritis: This autoimmune condition particularly impacts the joints in the hands and feet.- Celiac Disease: Individuals with this condition exhibit lifelong intolerance to gluten protein.
- Multiple Sclerosis: A chronic inflammation of the nervous system.
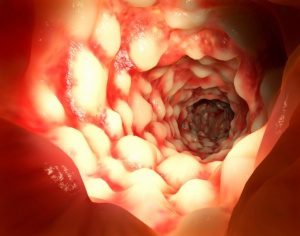
- Crohn’s Disease: A chronic inflammatory bowel disease.
Outlook: Implications Drawn from the Study’s Findings
The study authors emphasize the need for further research to delve into the relationship between endometriosis and autoimmune conditions.
The present study successfully established a connection between endometriosis and certain autoimmune conditions, yet this does not rule out the possibility of links with others. Additionally, it remains essential to determine whether endometriosis triggers autoimmune conditions or if both share common underlying causes, such as similar or identical triggers.
As mentioned earlier, a recent study [7] exploring the association between endometriosis and the autoimmune condition of rheumatoid arthritis (RA) provides insight into this matter. In this study, women with endometriosis were observed over an extended period, and it was evident that endometriosis did not appear to be a consequence of RA. This suggests a more plausible scenario where the autoimmune disease follows endometriosis or both conditions share a common cause.
The study’s authors urge healthcare providers to remain vigilant when patients present with relevant symptoms and are diagnosed with an autoimmune condition or endometriosis.
Summary:
Endometriosis, affecting a significant percentage of women of reproductive age, has remained a mystery in its cause. Recent research suggests it is a systemic condition, prompting a study examining the link between endometriosis and autoimmune conditions. This study revealed connections between endometriosis and at least 6 of them. Further investigations are needed to elucidate how these conditions interact, whether one triggers the other, or if they share common underlying causes.
References
- Diagnosis and therapy of deep infiltrating endometriosis
The Diagnosis and Treatment of Deep Infiltrating Endometriosis
Dtsch Arztebl Int 2010; 107(25): 446-55; DOI: 10.3238/arztebl.2010.0446
Halis, Gülden; Mechsner, Sylvia; Ebert, Andreas D. - https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(21)00389-5/
- https://pubmed.ncbi.nlm.nih.gov/31260048/
- Gynecology and obstetrics. Springer Verlag, 2006, ISBN 3-540-32867-X; excluding cancer.
- Ebert, Andreas D.. Endometriosis: A Guide to Practice, Berlin, Boston: De Gruyter, 2019.
- https://www.doccheck.com/de/detail/articles/32068-endometriose-eine-chronische-systemerkrankung
- https://pubmed.ncbi.nlm.nih.gov/33331948/
- https://www.rosenfluh.ch/media/gynaekologie/2012/03/pathogenese.pdf
- Endometriosis and Migraine: What is the Connection Between the Two Conditions? - 8. October 2023
- Endometriosis and Migraine: What is the Connection Between the Two Conditions? - 8. October 2023
- Can I Inherit Endometriosis? - 7. October 2023
