Watch out! Seven Must-Know Facts About Endometriosis!
Do you know what endometriosis is? No? Have you ever heard of it? Maybe, but you are not quite sure what it is all about? Then it is time you get the scoop!
It is a common condition. If it were a political party and the individuals with endometriosis were the voters, it would enter the Bundestag. And yet, it is still flying under the radar. Many people have never even encountered the word “endometriosis,” and even some doctors are not quite in the loop about the deal.
Yet, an estimated 10%-15% of women of childbearing age deal with endometriosis – over 2 million in Germany alone. Their quality of life suffers, and instead of getting the support they need, they often get shrugged off with remarks like, “Oh, it is just period pain; do not be dramatic!”
You, too, may have friends who go MIA during their periods, suddenly cancel plans, or skip work altogether.

Approximately 1 in 10 women of childbearing age is affected by endometriosis.
The impact on well-being and quality of life caused by endometriosis can rival other chronic diseases, such as cardiovascular conditions and certain cancers. Even more distressing is that it primarily affects young women, depriving them of what should be the prime of their lives! Adding to the burden, society, and regrettably, even some doctors, including gynecologists, contribute to the problem. Instead of understanding and support, they often ridicule those living with endometriosis, dismissing their pain and struggles with nothing more than a hot water bottle and a sneer.
I must confess that I, too, knew little about endometriosis before working as a doctor in the Endometriosis Center of the University Hospital. And to be quite honest – I knew nothing about endometriosis before I started studying medicine!
Through numerous conversations with friends, acquaintances, patients, and even strangers, I have realized that this lack of awareness is widespread. Shockingly, even many doctors know little about it.
This cannot continue!
Where Does the Ignorance About Endometriosis Come From?
What can we do to ensure that women with endometriosis are taken seriously?
While the reasons for this lack of recognition encompass historical, societal, and health policy factors, let’s now focus on the solution:
The most crucial step is to raise widespread awareness about endometriosis across our society. Knowledge about this cruel disease is the necessary foundation for fostering greater understanding, garnering more support from both the community and policymakers, boosting research initiatives, expanding treatment capacity, and ultimately leading to a better life for women with endometriosis.
Take just 5 minutes to learn about endometriosis – your efforts will be appreciated by all who are impacted by it.
So What Should EVERYONE Know About Endometriosis?
If everyone knew these seven facts about endometriosis, we would be one step closer to truly comprehending the challenges faced by women living with it!
Endometriosis is a chronic, benign condition where endometrial-like cells grow outside the uterus, commonly found in the abdomen (peritoneum, ovaries, pelvic walls, or diaphragm), but rarer cases may involve growth in scars, lungs, or the brain.
But it’s not just about the knowledge; it’s about empathizing with the profound impact it has on those affected!
1. Endometriosis Causes Pain – and It Has Nothing to Do With Normal Period Pain.

Experiencing severe pain during menstruation can be a potential sign of endometriosis
During a typical menstrual period, the uterus contracts, causing discomfort and cramps. Bloating may also occur a few days before. While this can be unpleasant, it typically doesn’t result in fainting or severe debilitation, allowing most women to carry on with their daily activities like shopping, working, or dancing at a party.
However, if the pain becomes unbearable, leading to bed rest, emergency room visits, fainting, or sitting hunched over in agony, it may be indicative of a more profound issue, often associated with endometriosis.
Endometriosis involves the growth of cells resembling the uterus in abnormal places, such as the ovaries, abdomen, pelvic walls, diaphragm, or even rarely in the lungs
Though its exact cause remains unclear, the effects are well-documented: inflammatory reactions, invasive growth into surrounding organs, and hormone-dependent bleeding, all contributing to pain and other related symptoms.
While not all women with endometriosis experience pain, it is the most common and prominent symptom associated with the condition.
2. Endometriosis Touches Every Aspect of Life

The severe pain often prevents women with endometriosis from participating in social activities.
Endometriosis profoundly impacts the lives of those affected on multiple levels.
Severe period pains can leave them tormented, causing them to miss work and social events, while relationships may also suffer. During periods of pain, women with endometriosis often find themselves adapting their entire lives to cope with the discomfort.
For many women, life is significantly altered on various levels. Severe period pains can leave them tormented, causing them to miss work and social events, while relationships may also suffer. Pain can extend beyond menstrual periods, persisting daily and affecting various aspects of life. Symptoms like pain during intercourse, fatigue, digestive issues, and discomfort during urination may arise. The condition may impact the ureter, leading to kidney congestion. Additionally, the presence of endometriosis near pelvic nerves can cause symptoms such as numbness, radiating pain, or burning sensation.
Deeply infiltrating endometriosis lesions can affect organs (e.g., ovaries), resulting in functional complaints.
3. Why Does It Take So Long to Diagnose?
The biggest factor is ignorance. Many women mistake their pain for normal period discomfort and believe that they are simply more sensitive to pain compared to their friends.
Moreover, some individuals don’t like to talk about it, confiding only in their family members. Due to the familial accumulation (endometriosis is not directly hereditary, but families with many individuals affected by it can be found), the symptoms may seem ordinary with mothers also unaware of the condition.
Furthermore, women seeking help from gynecologists or the emergency room due to period pain often face ridicule. This usually occurs due to ignorance rather than ill will.
So there is still a lot of education to be done to reduce the time it takes for accurate diagnosis!

Women usually visit multiple doctors before diagnosis.
The elusive nature of endometriosis presents a challenge in reaching a diagnosis. Women frequently seek opinions from multiple doctors before receiving a definitive answer. Due to the diverse range of symptoms, a comprehensive endometriosis center typically involves collaboration between gynecologists, colon surgeons, urologists, neurologists, and nephrologists to provide specialized care and a more accurate diagnosis.
4. Endometriosis Is Not a Mental Illness
It’s disheartening that many people, including more doctors than I would like, believe that endometriosis is a psychological or psychosomatic disease. However, this belief is fundamentally wrong!
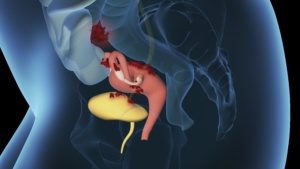
Endometriosis usually spreads in the abdomen. The cells resemble those from the uterine lining.
Endometriosis, a disease characterized by cells resembling the uterine lining, has an elusive origin yet to be conclusively determined. Lesions can manifest within the abdomen, peritoneum, and abdominal organs. In rare cases, they extend beyond the abdomen, affecting areas like the lungs, brain, or scars, leading to inflammation, pain, and functional restrictions, with varying symptoms based on their location.
Due to endometriosis lesions, recurrent surgeries, adhesions, nerve involvement, and the prolonged disease course, many women experience chronic pain. In some cases, the brain learns to produce pain independently of the stimulus, necessitating comprehensive care, including psychological support. However, it is crucial to emphasize that endometriosis is not a mental illness.
The extended duration of suffering, the above-mentioned associated health and social limitations, and limited treatment prospects can unfortunately contribute to the coexistence of psychological disorders. It is not uncommon for endometriosis to be linked to depression or other mental illnesses.
5. Endometriosis Complicates Pregnancies
Endometriosis is one of the most common causes of infertility, underscoring the importance of addressing it before embarking on fertility treatments. The intricacies surrounding this connection remain subjects of ongoing research, with factors like the inflammatory milieu, ovarian damage, and adhesions, such as those affecting the fallopian tubes, coming into play.
The unfulfilled desire to have children often results in significant limitations on both the quality of life and relationships. However, it is vital to note that many women with endometriosis can still conceive. Seeking guidance from specialized professionals at an endometriosis and fertility center can be immensely beneficial in addressing any questions or concerns in this regard.
6. What Does Not Help: Belittlement, Excessive Pity, Platitudes and Simplistic Advice

Women with endometriosis often hear a lot of well-intentioned but unhelpful generalized advice.
Women with endometriosis often encounter well-meaning advice, like:
- “It’s all in your head, why don’t you try meditation?”
- “It’ll go away!”
- “You just have to eat the right food, and it will go away on its own!”
- “Think positively”
While these words may carry some truth and good intentions, they oversimplify the complexity of endometriosis, which cannot be resolved with simple measures alone.
Meditation, nutrition, and positive emotions are indeed vital elements of multimodal pain therapy, which can yield good results. However, managing endometriosis is far from easy, and each woman requires a personalized therapy plan and a compassionate understanding.
The best course of action involves seeking treatment at an endometriosis center, where an individualized approach is developed. Alongside medical care, genuine sympathy and support from the environment play a crucial role in helping women cope with the challenges of endometriosis.
7. What Helps: Adequate Medical Treatment and Good Self-Management.
First, the good news: endometriosis is treatable.

The gold standard involves endometriosis surgery, preferably by excision, performed as a laparoscopy, or, in some cases, through an abdominal incision. Hormone therapy also proves helpful for managing symptoms.
However, the challenging aspect is that endometriosis can take a chronic course, attributed to recurrent lesions, incomplete surgery, or persistent pain
Therefore, experts repeatedly recommend multimodal pain therapy from the outset.
Nutrition, meditation, physiotherapy, massages, and more can significantly alleviate symptoms and improve chronic pain through cognitive changes.

In the treatment of endometriosis, the collaboration of experienced physicians and good cooperation between different specialties are essential.
The most important factors for successful therapy include:
- Experienced practitioners and surgeons: Seeking treatment from endometriosis specialists, consulting experts, and good cooperation between different specialties are essential!
- Active management of treatment: Since, unfortunately, symptoms may persist or reoccur during or after treatment and many pains have become chronic, women with endometriosis should empower themselves by seeking comprehensive information, making informed treatment decisions, and prioritizing their well-being. Active participation in their care has been shown to yield the best outcomes.
Conclusion
Endometriosis is a common condition that deserves awareness from every woman and man, including you! Even if you only read this section, here’s what you should remember:
- Endometriosis results from cells resembling the uterine lining, though its origin remains uncertain. Severe pain, particularly during menstruation, is the most prevalent symptom of endometriosis.
- The symptoms of endometriosis are varied, affecting various organs, and impacting women socially and professionally. So if a friend cancels a date due to severe period pain – don’t be angry, but think endometriosis!
- Late diagnosis is common, leaving many women unaware of their condition.
- Endometriosis can affect your mood and psyche, but endometriosis is NOT a psychological condition. Women with endometriosis are not imagining their pain. It is a real medical condition.
- Endometriosis can complicate pregnancies, prompting the need for clarification in cases of an unfulfilled desire to have children.
- What does not help: excessive pity, platitudes, trivialization, or simplistic advice.
- What helps: understanding from those around, treatment in specialized endometriosis centers, and a pro-active self-management of the disease and treatment.
You can get more help and tips for everyday life with endometriosis in the Endo-App. Download it to benefit from our expert knowledge.
References
- Current Research on Endometriosis: An Interview with Deborah Bush - 6. February 2024
- Pain and Pain Management – Interview with Rehab Psychologist Teresa - 19. November 2023
- Physiotherapy for Endometriosis – Interview with Annika Cost – with Exercises - 19. November 2023
